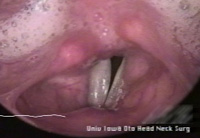
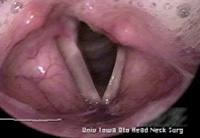
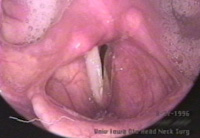
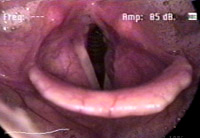
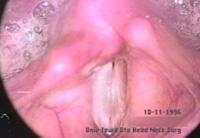
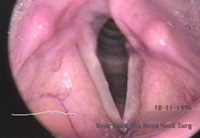
History 37 year old woman with an 18-year history of hoarseness. This hoarseness had a gradual onset at age 19 with deterioration of voice over a period of about 1 year. Since then, her dysphonia has been very stable. No other head and neck abnormality is noted with the exception of some tympanic membrane scarring, and an early childhood history of otitis. Initial examination The patient presents with a breathy voice, intermittent pitch breaks and roughness.
Operation The patient was sedated, and local anaesthesia obtained in the skin and deep structures overlying the left neck. A fibreoptic pernasal laryngoscopy was performed to confirm the left-sided paralysis. The patient's neck was strilely prepared and draped with the neck exposed. A six cm incision was made over the lower aspect of the thyroid cartilage along a wrinkle line. Subplatysmal flaps elevated superiorly and inferiorly while identifying th laryngeal prominence and cricoid cartilage. The strap muscles were separated in the midiline, and the posterior aspect of the thyroid perichondrium elevated. The muscular process of the arytenoid cartilage was then identified in dissection of the posterior larynx. A 4-0 prolene suture was placed through the muscular process. A thyoid cartilage window was designed 8 mm posterior to the midline and about 3-4 mm up from the inferior border of the thyroid. The cartilage window was removed using scalpel dissection and a drill to remove approximately 6x12mm of cartilage. The arytenoid sutures were brought forward through the window. A GoreTex implant was fashioned in a 5mm wide strip, and incrementally placed through the window while monitoring the patient's voice quality. In the process, excellent voicing was accomplished and a small amount of GoreTex added to ensure a slightly pressed voice (thus allowing for postoperative oedema to resolve to normal voice). The GoreTex was sutured in place with the sutures from the arytenoid muscular process, thus rotaing the arytenoid cartilages and ensuring posterior glottic closure. The larynx was again inspected using a fibroptic laryngoscope to check glottal approximation. The strap muscles, platysma and would were reapproximated with no complications. Total duration 1 hour 40 minutes. Postoperative Examination 1 At her three-week postoperative examination, the patient showed considerable improvement in the quality of her voice. The audio recording below demontsrates this improvement when compared to the preop audio recording. The patient's voice is mildly dysphonic, with only mild breathiness to report. No pitch breaks are noted, and no roughness. Maximum phonation time is up 11 seconds from 18 to 29 seconds.
Postoperative Examination 2 Three months postoperatively, the patient's voice has further improved. The posterior glottic chink and its associated breathiness have disappeared, and correspondingly maximum phonation time increased to 44 from 29 seconds. At this evaluation, the patient's voice is judged to be mildly dysphonic, with some roughness and no breathiness. Vocal fold vibration is symmetrical, and a healthy mucosal wave is seen on both vocal folds. Again, both vocal folds are seen to be smooth and straight. The oedema and erythma of the left ventricule has resolved.
|